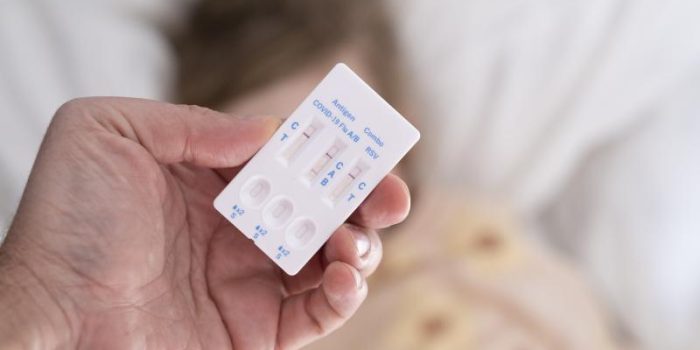
Use of rapid antigen diagnostic tests for respiratory syncytial virus (RSV) in young children was tied to significant reductions in RSV-linked antibiotic prescribing, researchers reported yesterday in JAMA Network Open.
RSV is a significant cause of viral lower respiratory tract infections (VLRTIs) in children, including 50% to 80% of children five years old and younger who are hospitalized with bronchiolitis and 40% of those over 12 months who are hospitalized with pneumonia. Yet, despite established guidelines that emphasize antibiotics provide no therapeutic benefit, RSV-related in children is frequently treated with antibiotics, particularly in doctor’s offices and other outpatient settings where access to diagnostic testing that can differentiate between viral and bacterial infections is limited.
But in the wake of the COVID-19 pandemic, which saw widespread uptake of rapid diagnostic tools, adoption of rapid tests for diagnosing RSV has grown. Using data from an independent network of more than 200 family pediatricians in Italy, a team led by researchers from University of Milan-Bicocca assessed the use of combination COVID/Flu/RSV rapid antigen diagnostic tests (Ag-RDTs) in infants aged nine to 36 months with suspected VLRTIs, including bronchiolitis. The primary outcome of the study was whether use of Ag-RDTs was associated with reduced antibiotic prescribing in children who test positive for RSV.
“These tools aim to improve diagnostic accuracy and potentially reduce unnecessary antibiotic use,” the study authors wrote. “Although rapid tests are increasingly adopted in pediatric settings, evidence of their association with antibiotic prescribing for children in community settings remains scarce in the current literature.”
Antibiotic prescriptions nearly cut in half
Among 256 children (median age, 15 months; 52% male) enrolled in the study, 79 (30.9%) tested positive for RSV and 177 (69.1%) were RSV-negative. Antibiotic prescribing was lower in the RSV-positive than RSV-negative children (0.18 prescriptions per 10 person-days vs 0.29). Detection of RSV by Ag-RDT was associated with a 48% reduced risk (relative risk [RR], 0.52) of receiving at least one antibiotic prescription.
When the researchers compared antibiotic prescribing in matched cohorts with clinically diagnosed VLRTIs in the 2023-24 and 2022-23 seasons, they found Ag-RDT implementation was associated with a 39% (RR, 0.61) and 46% (RR, 0.54) lower risk of antibiotic therapy, respectively.
“This cohort study of 256 children highlighted the potential of RSV Ag-RDTs to reduce inappropriate antibiotic prescribing for LRTIs in pediatric community settings,” the authors wrote. “By improving diagnostic accuracy at the point of care, Ag-RDTs can support more targeted treatment decisions and strengthen antimicrobial stewardship.”
The authors add that larger studies are needed to confirm the generalizability of the findings and the cost-effectiveness of Ag-RDT implementation.
By improving diagnostic accuracy at the point of care, Ag-RDTs can support more targeted treatment decisions and strengthen antimicrobial stewardship.
In a commentary that accompanies the study, Carl Llor, PhD, of the University of Southern Denmark, writes that while the study “represents an important step forward in advancing our understanding of the impact of rapid RSV testing on antibiotic prescribing in primary care,” the small size of the cohort and the inability to account for disease severity—which can influence prescribing decisions—limit the findings.
“The findings suggest that virologic confirmation can increase clinicians’ confidence in withholding antibiotics when a viral etiology is identified, thereby supporting more judicious prescribing practices, particularly in nonserious cases,” he wrote. “However, the role of RSV testing in more severe presentations remains uncertain.”