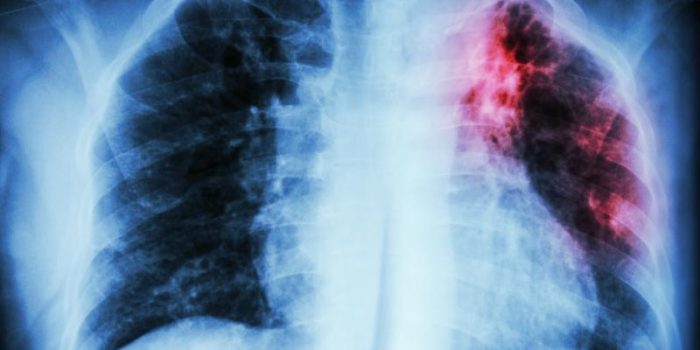
The results of a phase 3 trial conducted in India reveal that two experimental tuberculosis (TB) vaccine candidates did not show efficacy against all forms of TB but were safe and offered limited protection against a more severe form of the disease.
The PreVenTB trial, conducted from July 2019 to December 2020 by a team led by investigators from the Indian Council of Medical Research, involved 12,717 household contacts of recently diagnosed TB patients in six Indian states. Participants were randomly assigned 1:1:1 to receive an injection of either of the vaccines—VPM1002 or Immuvac—or placebo in both arms, followed by a second dose a month later. The primary outcome was efficacy against confirmed TB (pulmonary and extrapulmonary TB) over 38 months of follow-up.
VPM1002 and Immuvac are two of 16 vaccine candidates in the pipeline for TB, which sickened an estimated 10.7 million people and killed 1.2 million globally in 2024. The only licensed TB vaccine, bacille Calmette-Guerin (BCG), has been widely implemented in national immunization programs and protects young children against extreme forms of TB but is not effective in adolescents and adults.
India has one of the highest TB burdens in the world. The 2.6 million cases reported in 2024 accounted for 25% of the global total.
“The efforts to achieve TB elimination by 2025 include early detection, treatment, and prevention of disease in the most vulnerable people,” the trial investigators wrote last week in The BMJ. “Although India has adopted TB preventive treatment, additional strategies like prophylactic vaccines are required.”
Protection against extrapulmonary TB
Neither vaccine provided protection against all TB, pulmonary TB, and latent TB. But VPM1002 showed a vaccine efficacy (VE) of 50.4% against extrapulmonary TB, which occurs when TB spreads beyond the lungs, and Immuvac had a VE of 33.2% against extrapulmonary TB. VPM1002 and Immuvac showed VE of 64.9% and 66.3%, respectively, against extrapulmonary TB in participants with tuberculin skin-test positivity.
“Extrapulmonary TB, which occurs at sites other than the lungs, occurs in about a third of patients diagnosed as having TB, and the mortality for this form of TB may increase to about 40% in some countries,” the investigators noted.
VPM1002 also demonstrated VE of 64.6% for all forms of TB, 62.1% against pulmonary TB, and 77.6% against extrapulmonary TB in children aged 6 to 14 years, while Immuvac provided protection against extrapulmonary TB only in children aged 6 to 10 years. The confidence intervals for all VE estimates, however, were wide, indicating considerable uncertainty, and the ranges for several dropped below zero, indicating findings that aren’t statistically significant.
Neither vaccine provided protection for children who were underweight. Both vaccines were well-tolerated and induced an immune response.
Though the vaccines did not provide protection against all forms of TB, the investigators say the reduced incidence of extrapulmonary TB in all age-groups, and the efficacy in children are findings that policy makers should consider.
“The data showing protection from pulmonary TB in a younger age group and from extrapulmonary TB in general will help to reduce the burden of TB,” they wrote.